Dr. Xinyu Zhao of the Waisman Center and Department of Neuroscience at University of Wisconsin-Madison joins us in this seminar to present Interrogate the Functions of FMRP in Brain Development Using Stem Cells.
Read morematrix metalloproteinase
Mechanisms and Biomarkers of Sensory Hypersensitivity in the fmr1 Knockout Mouse

In this Fragile X research webinar we hear from Devin K. Binder, MD, PhD, Professor, University of California at Riverside Medical School and Khaleel Razak, PhD, Professor, University of California at Riverside as they present about Mechanisms and Biomarkers of Sensory Hypersensitivity in the fmr1 Knockout Mouse.
Read moreClinical Trial of Metformin for Fragile X Syndrome

Metformin is commonly prescribed to control high blood sugar in type 2 diabetes. With a $50,000 grant from FRAXA Research Foundation, Dr. Artuela Çaku and Dr. Francois LePage are conducting an open-label clinical trial of metformin for children and adults with Fragile X syndrome, at the University of Sherbrooke in Canada.
Read moreUnderstanding and Reversing Hypersensitivity to Sounds in Fragile X Syndrome

With a $90,000 grant from FRAXA Research Foundation over 2018-2019, Drs. Devin Binder, Iryna Ethell, and Patricia Pirbhoy at the University of California at Riverside aim to understand – and reverse – hypersensitivity to sound in Fragile X syndrome.
Read moreCombinatorial Drug Treatment in a Model of Fragile X Syndrome using Novel Biomarkers

With a $90,000 grant from FRAXA Research Foundation awarded over 2016-2017, University of California researchers Khaleel Razak, PhD, and Jonathan W. Lovelace, PhD, are exploring drug combinations to limit hypersensitivity to sounds in Fragile X mice.
Read moreMetformin, Diabetes Drug, Potential Fragile X Treatment

“We treated mice with metformin and corrected all the core Fragile X deficits. We are optimistic about using metformin in human clinical trials. This is a generic drug with few side effects” says Nahum Sonenberg, PhD, James McGill Professor, Department of Biochemistry, McGill Cancer Center, McGill University.
Read moreRepurposing Available Drugs to Treat Fragile X Syndrome – FRAXA Initiatives
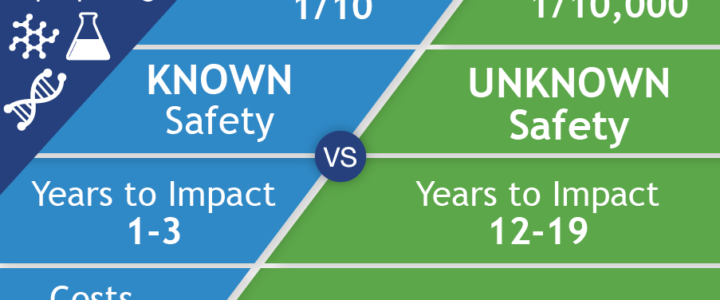
FRAXA Research Foundation was founded in 1994 to fund biomedical research aimed at finding a cure for Fragile X syndrome and, ultimately, autism. We prioritize translational research with the potential to lead to improved treatments for Fragile X in the near term. Our early efforts involved supporting a great deal of basic neuroscience to understand the cause of Fragile X. By 1996, these efforts had already begun to yield results useful for drug repurposing. To date, FRAXA has funded well over $25 million in research, with over $3 million of that for repurposing existing drugs for Fragile X.
Read moreFragile X Syndrome Treatment Target: MMP-9

Dr. Ethell was awarded FRAXA Research Foundation funding from 2008-2011 and 2012-present. This latest work shows that human Fragile X tissues have elevated levels of the extracellular enzyme MMP-9, as well as an increase in the active fraction of that protein (like most enzymes, MMP-9 can exist in an inactive form which can be switched on rapidly; this kind of regulation is important in most biological pathways.)
Read moreMatrix Metalloproteinase Therapeutic Treatments for Fragile X Syndrome

With a $157,000 grant from the FRAXA Research Foundation in 2012-2013, Dr. Kendal Broadie and Dr. Cheryl Gatto worked to define the distinct but also overlapping roles for MMP-1 and MMP-2 in synaptic structural and functional development. In drug studies with Fragile X fruit flies, they will be testing a range of MMPIs in drug treatments to compare effectiveness during development and at maturity, in order to define the contributions of FXS developmental impairments and adult recovery/plasticity.
Read moreEffects of minocycline on vocal production and auditory processing in a mouse model of Fragile X

With $135,000 in grants from FRAXA Research Foundation over several years, Dr. Khaleel Razak and Dr. Iryna Ethell explored robust biomarkers relevant to the FXS and the efficacy of minocycline treatment.
Read moreEncouraging Results from First Trial of Minocycline in Fragile X

With a $40,000 grant from FRAXA, Dr. Carlo Paribello and his team at the Surrey Place Centre Fragile X clinic in Toronto, Ontario, ran an open label trial to see if minocycline can improve learning and reduce anxiety and behavioral problems in people with Fragile X. Twenty participants between the ages of 13 and 35 years took minocycline for two months.
Read moreRole of Matrix Metalloproteinases (MMP-9) in Fragile X

With a $220,000 grant from FRAXA Research Foundation over 3 years, Dr. Iryna Ethell from the University of California at Riverside studied the regulation of dendritic structure by matrix metalloproteinases and other extracellular signaling pathways. This work identified a major treatment strategy for Fragile X with the available MMP-9 inhibitor, minocycline.
Read moreResearchers Propose Minocycline to Treat Fragile X

A University of California Riverside team of scientists has found that an available drug called minocycline, used widely to treat acne and skin infections, might also be used to treat Fragile X. The study’s findings have already led to the approval of a FRAXA-funded clinical trial in Toronto, Canada, that will test minocycline in patients with Fragile X.
Read more
